When I woke up on the third morning after my mastectomy, something felt different, and it wasn’t immediately clear why. I was still nestled in a white padded vest that I’d been intricately hooked into like a 19th-century courtesan. I was still propped up in bed, clouded by a collection of medications I would never learn the names of, flanked by cats who learned early that I could be counted on now as a consistent source of warmth. It wasn’t until I stood up—much to the chagrin of the cats—that I was greeted with a sudden clarity. There was a stirring in my body that I could suddenly feel. Somewhere, under the layers of padding and iodine and gauze and surgical glue, was the chest that I’d been visualizing and manifesting since long before I understood why.
Carefully, tenderly, I pawed at the collar of the sleeveless straitjacket my surgeon had made me promise not to touch for the first week of my recovery. For two nights now I had been plagued by dreams of medical disaster. In my nightmares, I woke up in recovery rooms with an unchanged body, surgeons apologizing for the mix-up, sending me home, promising to keep in touch with updates before vanishing forever. I dreamed of missed chances, of postponed care, of disapproving nurses, and in one case, of a poorly attached nipple dislodging completely, lost forever down a shower drain.
These anxieties and my deep need to follow the exact letter of my surgeon’s instructions gave me pause for just a moment before I gave in to curiosity. With the four inches of stacked geometric padding temporarily freeing my tender chest, I glanced down.
They were gone.
Euphoria flooded in.


It wasn’t cute down there. My nipples were still shrouded by quarter-sized gauze pads that had been stained dark. My incisions, twin half-moons that stretched from an inch below my armpit to the center of my sternum in a half-yard of angry red stitching, were accented by blossoming bruises in a variety of alarming colors. But none of that mattered: A part of my body that had always been stranger to me, that made me feel like a visitor in my own vessel, was a memory now.
First I grinned. Then I cried.
Twenty years of weight melted off of me. I was still weak and tired and drained, unable to grip a glass of water or use my arms to prop myself up in bed, but I was happy. It would still be a week or two before I could put on a cotton t-shirt and run my hands down my front, marveling at the miracle of my reflection, longer still before I would see all of myself at once and recognize completely the person looking back at me, but in that moment, I was in complete peace. I settled under my blankets, cats chirping their approval, and fell back asleep shrouded in bliss.
—
The long name for my surgery is “bilateral mastectomy for transgender chest recontouring with free-nipple grafts” but in the trans community, we just call it “top surgery.” Though these kinds of surgeries have existed for almost a hundred years—with the first patient recorded as seeking gender affirmation this way in 1945—they’re still tragically challenging to access today, especially for those of us in the community who face the extra hurdle of not fitting into the gender binary.
Twenty years of weight melted off of me. I was still weak and tired and drained, unable to grip a glass of water or use my arms to prop myself up in bed, but I was happy.
To be nonbinary means to be constantly pushed into corners we are actively rejecting. Even in my own surgery notes, only minutes after my nurse completed my intake paperwork using “she/her” like her life depended on it, I am referred to as a “female to male” trans patient, and regarded as “he” for four pages of medical play-by-play. Even when they get it right, they still get it wrong.
This kind of near-miss medical care isn’t just personally frustrating, it has real consequences. Even within queer communities, it can be challenging to convince well-meaning people to divorce themselves from binary thinking, clouding any chance at understanding why we are also deserving of gender-affirming healthcare. When recovering from my own surgery, I reached out to another nonbinary friend of mine who is almost seven years healed from the same procedure to see if that feeling had any truth to it.

“I didn’t start exploring the gender binary until I was safely away from my own dysphoria,” they tell me. “I was identifying as a binary trans man then, and pursuing medical transition was probably easier that way.” Sam, who is a 27-year-old Southern California native, says that they feel lucky to have navigated the “unending pointless bureaucracy” of surgery early, but they did suffer the sting of medical gatekeeping and binary understandings of gender even then. “A therapist at my LGBT center asked if I liked to do ‘boy things’ as part of my dysphoria diagnosis,” they remember. “She had a very black-and-white view of gender, and wouldn’t call me ‘he’ until I started on hormones.”
This question of who is “trans enough” to be trans isn’t new in our community. It’s called transmedicalism, and it’s rampant in conversations about the access and necessity of our surgical interventions. For every person on the outside who is worried that we’re being pushed into surgery, there’s someone arguing that we aren’t who we are without it.
To be nonbinary means to be constantly pushed into corners we are actively rejecting.
This, of course, is the highest form of absurdity, and it’s often coupled with the belief that every transgender person who pursues surgery feels they were born in the “wrong” body. My body was never wrong, it just felt like it wasn’t sized quite right. I didn’t hate it, it just didn’t fit, like borrowing a pair of jeans that were custom tailored for someone else. “I couldn’t find the joy in my body,” Sam agrees, “but it was still mine.”
So why do it?
Why subject ourselves to a year of waiting, to therapist appointments, to blood tests, to letters of recommendation, to surgery consultations, to fundraising, to steep co-pays, to medical prejudice, to anesthesia, to physical trauma, to weeks of weakness and exhaustion and pain?
“Surgery felt like an act of self love,” Sam tells me. And I agree.

A week after I woke up in recovery—throat sore from intubation and chest bound tight in bandaging—it was time to take the vest off. Not forever, my surgeon warned me: I would still have to wear the outermost layer of the vest, would still have to navigate the endless row of tiny hooked clasps with hands that could still barely grip toilet paper, but I would be free from the padding that obscured my new silhouette. I told him about the nightmares. “I’ve performed this surgery hundreds of times,” he said, not looking up from a steady stream of notes he was typing into a laptop in the corner of the exam room, “and I’ve never lost a nipple.” So I should be able to shower without fear, which was nice.
A moment later, my surgeon promising to return with instructions for the next few weeks and some fresh bandages in a moment, I faced my own reflection in a small mirror mounted behind the door. I undid each hook, frightened again that something might have gone wrong. A side effect of the surgery that I was most unprepared for was the near-universal numbness that spread from my diaphragm to the base of my throat. Some of the feeling was returning, but not all of it, especially along my scar lines. If something was wrong or disfigured, it would be tough to tell under all of the layers. And with my first peek at home days before, I had only seen my chest from above. What if my belly, now inarguably the most prominent part of my torso, presented me with a brand new kind of dysphoria?
The last clasp undone, I cracked the vest open like a Maine lobster and let the garment fall past my elbows. I turned to the side, my hand hovering over my incisions, still too scared to touch them. I looked at myself from behind, craning my neck to catch a glimpse over my shoulder. I raised and lowered my arms, and met my own eye line, blinking away tears I didn’t know were there.
“Oh my god,” I whispered to myself, “there you are.”
The hard knocking of my surgeon at the door snapped me out of it. “No!” he gasped, jogging in with a nurse at his heels. “I missed it! It’s my favorite part!”
—
Adler, another arm of the trans-masculine community that I’ve been steadily growing over the last decade, is a few years younger than Sam and I, but has memories of early gender questions that are eerily similar to our own.
“I had no examples of what it meant to be trans and nonbinary,” they tell me, “I was called a tomboy growing up. I competed against boys to win and earn their approval, but when you don’t see examples of something and there’s no representation, it just doesn’t exist. There was no alternative.”

The language for nonbinary identity, for what it means to be trans in a way that is not clearly one version of gender or another, has made it hard for all of us to find medical care. Adler’s experience has been particularly frustrating. “A lot of people still see gender as binary. They have sexuality handled as a fluid space with room for a spectrum, but not gender.” They, too, have felt the sting of unclear pathways to surgery. “I got a lot of nos from healthcare providers in my area,” Adler explains, “no one could help me or point me in the right direction, and it became very discouraging. There was a very low return on the time and energy I was putting into it.”
For many trans people seeking surgery, me included, the first step toward a surgical consult is usually a meeting with a therapist who can diagnose us with gender dysphoria. The easiest way to understand dysphoria is this: it is a mismatch between the gender we are assigned at birth and our own internal sense of our gender. For most people, the two line up, like a set of matching memory game cards. For some of us, we get the yellow star and a blue heart, which means it’s time to flip the cards and draw again.
The hardest way to understand it is the way championed by my insurance-assigned therapist. Trans people are usually assumed to have access to much more sophisticated language concerning their experience with gender than cisgender people. When the first step to gaining access to an often life-saving medical procedure is being able to explain my experience with gender like a PhD candidate defending a psychology dissertation, there is a gap in accessibility that needs to be addressed.

So, imagine for a moment, sitting in a hot parking lot after a day of work, having barely connected to a video call with a therapist who will be calling back three more times over two months, trying to solve the riddle that will unlock the diagnosis that determines the future of my medical care.
Here are the questions she asked me, taken word-for-word from my medical record:
- What is your connection between your physical body and your experience with gender?
- Do you have a strong desire to be seen as your gender? Describe this desire.
- How long have you understood yourself as your gender? Describe this experience.
- Describe your relationship with your secondary sex characteristics (the characteristics that developed in your body after puberty.)
- Do you have a strong desire to be treated as a gender other than the one you were assigned at birth?
- How would a change in your physical body change your life?
- Do you have a strong conviction that you have the typical feelings and reactions of your true gender?
It’s hard enough to answer those questions from a cisgender perspective—there are countless subtleties and nuances that go into how we see ourselves and our bodies, and it’s harder still as a binary trans person, who will have to untangle how they were socialized against their will with how they feel and experience gender genuinely. But as a nonbinary person for whom even the idea of gender feels kind of like a scam? It’s even more fraught.
Adler, Sam, and I (along with the team who designed these questions) also come from a perspective that centers white and European ideas of gender. Our experiences are based around that reality, which is not the same for people who are Black or Brown or Indigenous, or who come from any place on earth other than our pocket of reality in a relatively permissive part of the United States.
“Sometimes I wonder if the world I was born into was different if I would need surgery to feel at home in my body.” I nod as Adler explains a feeling I’ve returned to over and over again throughout this process. “So much would have to change. Gender would have to not exist.”
—
There are surprising positives to the process, separate from a reformed version of a body that I can finally recognize. The upside of a surgery that renders my body in need of support is the chance for a community to show up and prove why so many of us have expanded our definitions of family. My roller derby team made a schedule of visitors on a spreadsheet, brought me and my wife meals, vacuumed our floors, and emptied our litter boxes. My wife, in her infinite love and generosity, sat at my bedside for a week, watching home improvement shows and feeding me fajitas. Where I once feared that my surgery could drive a wedge in our relationship, it has only bloomed.
“I stayed with my parents for a week or two,” Sam told me. It had been rocky at the start, when they first came out to their family as transgender when they were only sixteen. “I’m sure it’s hard, as a parent who doesn’t know anything about what it means to be trans and you have a teenager who tells you they are.”
“I see a path now from where I am to where I want to be.”
But surgery did something surprising for Sam: it brought them and their mother much closer. “It felt really special to have her care for me. She had me make a grocery list before and brought me acai bowls. We rented weird movies. It felt like she was supporting me and seeing me as I was. The first time she helped me shower she seemed scared of what I would look like, but then she said I looked like a rock star.”
For Adler, who is still just at the beginning of their top surgery journey and is still a couple of weeks away from their first recommendation letter, community is what has gotten them this far. “At first, I thought who could love me? Who could accept me? I just wasn’t seeing trans and nonbinary folks experiencing joy.” It was a roller derby team, the same one that made the spreadsheet, that started changing things for them. “I felt myself blossom. I went from maybe 40% sure of myself to 80%.” And a move to a more progressive part of our state didn’t hurt. “There’s a beautiful community here where gender-affirming care is a lot easier to come by.” And so the world starts to look a little brighter for Adler too.
“I see a path now from where I am to where I want to be.”
—
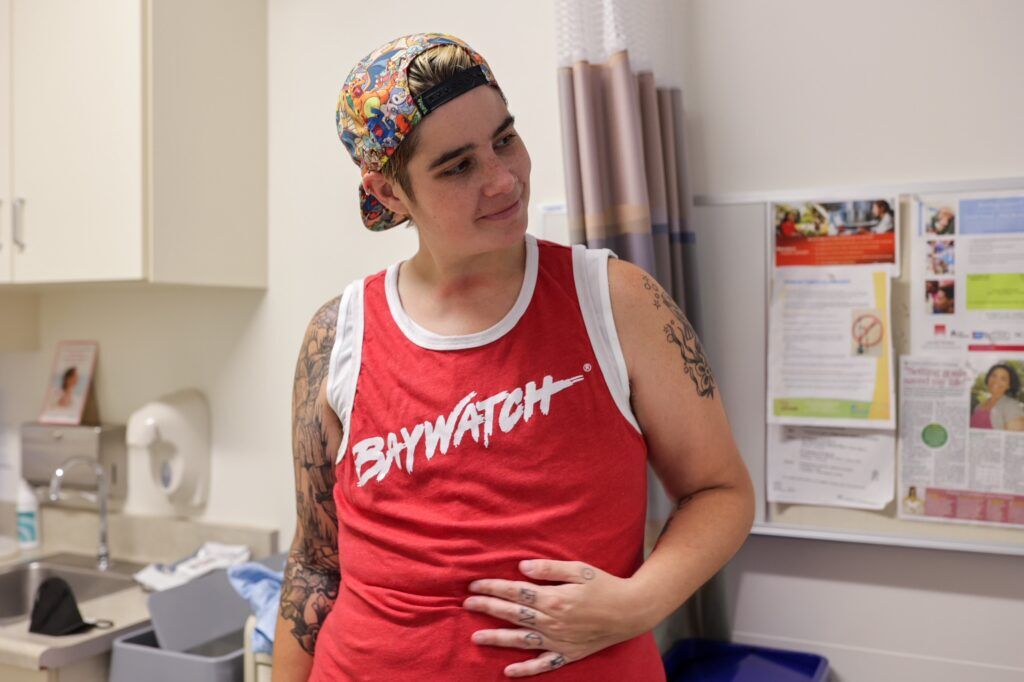
It’s been a month now since my procedure.
Bandages are gone, gauze is replaced by silicone scar care tape, laid gingerly over shiny pink tissue that I can massage with an open palm. My nipples have not fallen off, and now seem secure inlaid in a chest that feels like the morning after a particularly intense day on a bench press.
Catching my reflection is still startling, and I have to remind myself to skip the part of my morning routine where I reach for the small black binder and sports bra that were so habitual for so long.
Sweatshirts, layers, and baggy t-shirts have been replaced by button-ups that I leave undone down to my middle, muscle tanks, and a surprising number of crop tops. It’s the end of summer in Southern California, and my body is finally positioned to take full advantage. This part of the process, Sam tells me, where I’m constantly aware of how my body looks and moves, lasts a while. When they started to feel healed enough, their first stop was Target’s men’s section, for a pack of plain white t-shirts. “They never looked right over a binder,” they tell me.
But now, years later, they don’t think about it much anymore. “Now when I’m worrying about my body, I want to learn more about what it can do.”
Adler, for their part, also wants to know more about their body’s potential. “I’m so excited to see my chest muscles. I’ve been working on them with a renewed dedication and it would be nice to go running and not wear a sweatshirt.” Rightfully, Adler doesn’t try to exercise in a binder. Binding—though affirming—has to be done correctly to avoid potential danger. Even wearing one sized a bit too small for just a couple of hours too long cracked one of Sam’s ribs as a teenager.
Leaving concerns like that in my rearview mirror is just one of the many joys wrapped up in making this choice for myself. The decision to pursue surgery, Adler, Sam, and I agree, is easy to call extreme from someone who will never have to think about things like that.
“Cisgender people really just take the comfort of living everyday life for granted,” says Sam. “They get to just slip on their clothes and live their lives.” I wonder out loud when that will happen for me. When getting dressed won’t hold any kind of power over me one way or another.
Sam smiles. “There’s a reason I don’t think about my body much anymore.”♦
Don't forget to share:
Help make sure LGBTQ+ stories are being told...
We can't rely on mainstream media to tell our stories. That's why we don't lock our articles behind a paywall. Will you support our mission with a contribution today?
Cancel anytime · Proudly LGBTQ+ owned and operated
Read More in Culture
The Latest on INTO
Subscribe to get a twice-weekly dose of queer news, updates, and insights from the INTO team.
in Your Inbox













